Swallow
- Rachel Coates, Speech and Language Therapist
- 9 minute read
- Last updated: September 2023
Approximately two-thirds of stroke survivors will experience difficulty swallowing, also known as dysphagia. In many cases, it will resolve in the first few weeks after stroke, but it can cause long-term difficulties. The severity of the swallowing difficulties depends on the area of the brain affected by the stroke.

Swallowing

Swallowing is a complicated task – your brain has to coordinate many different muscles to do it. If your stroke damages the parts of your brain that manage this, then your ability to swallow will be affected.
Other effects of stroke can make eating, drinking and swallowing challenging.
Effects of stroke
Facial weakness
Lip and tongue weakness can cause difficulty with chewing and lip seal, so fluids or food may escape from the mouth.
Upper limb weakness
This can make it difficult to hold a cup or spoon and feed yourself and present challenges with preparing food.
Fatigue
Tiredness and difficulty concentrating can have an effect on swallowing.
Sitting balance
If your balance has been affected, you may not be able to sit up straight, which can make swallowing more difficult.
Stages of swallowing
There are four stages to swallowing. A stroke can affect any one of these stages.
Step 1
You see and smell food and put it in your mouth. You then prepare it for swallowing by adding saliva, chewing and moving it around your mouth.
Step 2
You close your lips, and your tongue moves the food or drink to the back of your mouth.
Step 3
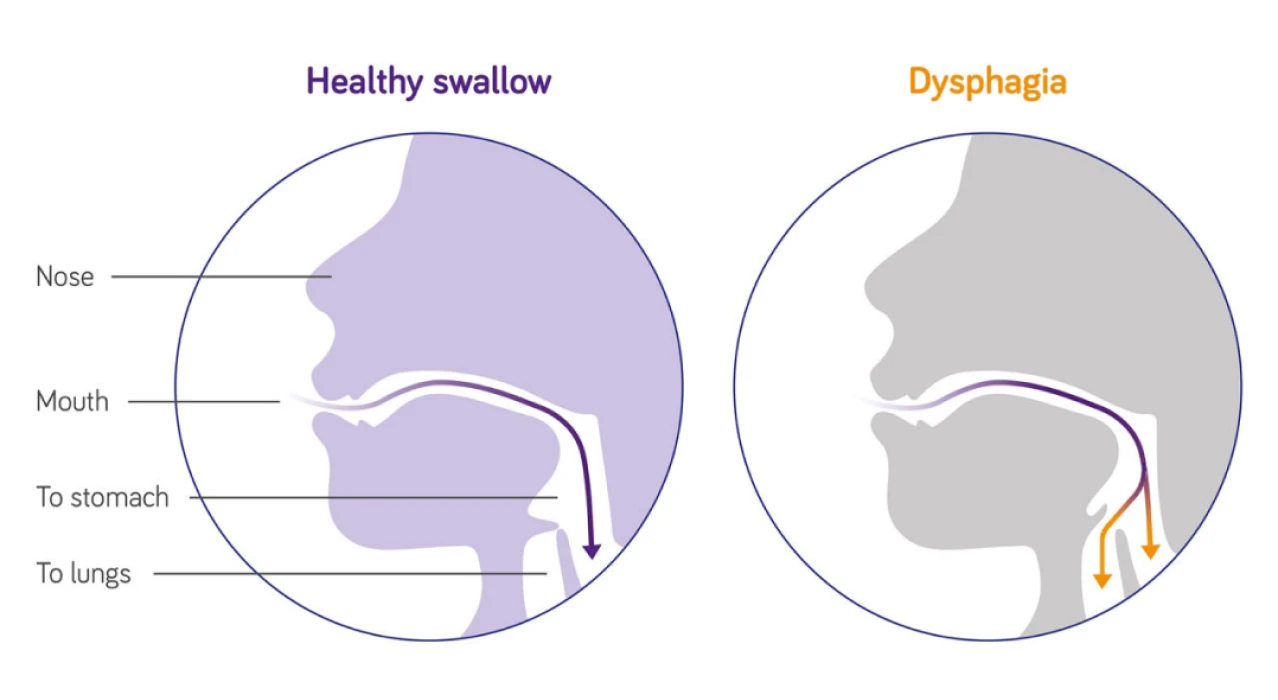
The food or drink moves through your throat to your food pipe (oesophagus), which carries food to your stomach. At the point of swallowing, a flap in your throat (the epiglottis) moves to close over and protect your airway (trachea), and your vocal cords close. This stops any food from going into your lungs.
Step 4
The muscles in your oesophagus squeeze to move the food down into your stomach. This is known as peristalsis.
Complications of dysphagia
If swallowing is impaired then food, drink and saliva may “go down the wrong way” and get into your lungs. This is known as aspiration and can lead to a serious lung infection called aspiration pneumonia. Signs of aspiration pneumonia include a high temperature, cough (sometimes with green or yellow sputum) and difficulty breathing/shortness of breath.
If you are not managing to eat and drink enough, swallowing difficulties can lead to weight loss and dehydration. It is important that any change to your swallowing is spotted early to stop this from happening.
If you notice that you are losing weight, speak to your dietitian, speech and language therapist, stroke nurse, or GP (family doctor).
Swallowing difficulties
Swallowing problems are not always obvious. It is good to know what to look out for. Sometimes food and fluids can go to down the “wrong way” and into the lungs without any obvious signs. This is known as silent aspiration.
Signs of swallowing problems
- Coughing or choking when you are eating or drinking
- Throat clearing when eating and drinking
- A “wet” sounding voice
- Shortness of breath when eating and drinking
- Bringing food back up, sometimes through your nose
- Feeling that food or drink is going down the wrong way
- Feeling that food gets stuck in your throat
- Not being able to keep food or drink in your mouth
- Still having food or drink left in your mouth after you have swallowed
- Not being able to chew food properly
- Saliva escaping from your mouth
- Taking a long time to swallow or finish a meal
Assessment
Everyone who has had a stroke should have a swallow screen carried out shortly after arriving at hospital. You should not have any food, drink or medications by mouth until your swallowing has been assessed. (This is often referred to as NPO or nil per oral.) If any difficulties are identified, then you will be referred to speech and language therapy for further assessment, which may include testing the cough reflex.
Sometimes instrumental assessments will be carried out by the speech and language therapy team. Some of the assessments that may be done are listed below.
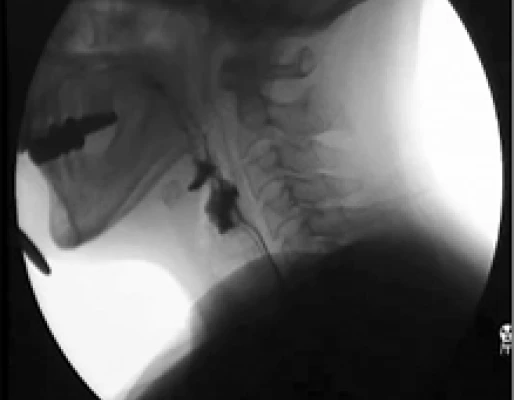
Videofluoroscopy
A video x-ray of the mouth and throat while you swallow different foods and drinks mixed with barium (so that they show up on x-ray).
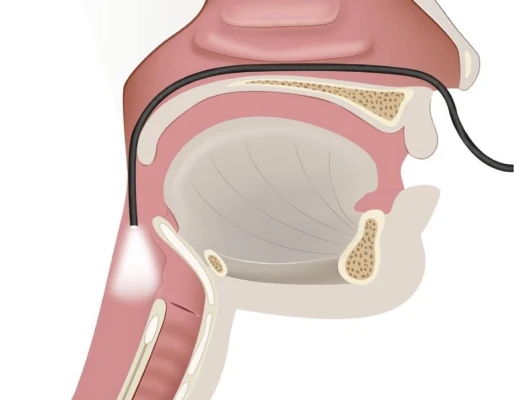
Flexible endoscopic evaluation of swallowing
Also known as FEES, this involves inserting a small camera through the nose and into the throat to look at how well the muscles are working. You will be given food and drink to swallow while the camera is inserted.
Will my swallow improve?
Most people will find that their swallowing difficulties get better within two weeks. A small number of people continue to have difficulties for longer than this. It may take some time to adjust to changes that need to be made. After an assessment, your speech and language therapist will be able to advise you on how to manage and improve your swallowing difficulties.
Swallow advice
- Change the consistency of your diet and fluids.
- Learn techniques that can help you to swallow.
- Use aids that can help you to eat or drink more easily.
- You may be considered for Pharyngeal Electrical Stimulation (PES) to treat sensory dysphagia if indicated.
Your speech and language therapist may also get you to do exercises to strengthen the muscles in your throat, face and mouth. This may help you to swallow better and protect your airway.
Adjusting diet and fluids
If you can’t swallow safely, then you may need to make changes to the consistency of your drinks and the texture of food you consume. Your speech and language therapist will advise you on this.
Thin liquids can be difficult to swallow because they travel quickly, and you may not have time to close your airway to swallow. Your therapist might recommend using thickened drinks to help you drink safely. This slows down the transit of the liquid. Thickened drinks are prepared using a powder which is added to liquid to achieve the right consistencies for safer swallowing. More information about the different consistency levels can be found here.
If you have problems with chewing and swallowing, you may need to change the type of foods you eat. There are different categories of food softness – from soft and bite-sized through to liquidised. Your speech and language therapist can advise you on the right texture for you and let you know which foods are safe to eat.

Tube feeding
If it is not safe for you to eat and drink, or if you are not able to eat and drink enough, then you may be offered a feeding tube. Tube feeding means putting liquid food directly into your digestive system through a tube. This is also known as “enteral feeding”. You might only need it for a short time if your swallowing improves, but some people will need it for longer.
There are different types of feeding tubes. The two that are used most often after a stroke are nasogastric (NG) tubes and percutaneous endoscopic gastrostomy (PEG) tubes. NG tubes go through the nose into the stomach. They tend to be temporary and are normally used if you will need to be tube fed for less than four weeks.
PEG tubes are inserted into the stomach through a hole in your skin. They tend to be used for longer periods. After some time using an NG tube, you may start thinking about changing to a PEG tube. You will need to talk through both options with your stroke team and your family to decide which one is best for you. There are advantages and disadvantages to both.
Your dietitian will provide you with a nutritional care plan to ensure you meet your nutritional needs whilst using your tube.
Other information
Top tips
Supporting someone with eating and drinking
Don’t give them food or drink if they are feeling tired or drowsy. Don’t rush them or offer too much at once. Don’t move from one food to another without asking them.
Rachel Coates | Speech and language therapist |
Presentation matters
Try to present food so it looks nice, and be positive and encouraging when you offer it. Keeping food separate on the plate is much more appetising than mashing it all together. Food molds can also help you to present pureed food nicely.
Rachel Coates | Speech and language therapist |
Frequently asked questions
Medications come in different forms, including liquids and patches. If you are struggling to swallow tablets, speak to your doctor or pharmacist to see if your medication comes in a different form that may be easier for you to take. Always check with your pharmacist first before crushing tablets, as this can change the way some medications work and can even be dangerous.
Just because you have swallowing problems, it doesn’t mean you can’t enjoy eating. If you are missing your favourite meals and snacks, speak to your speech and language therapist or dietitian. There may be a way for you to have them or to enjoy something similar. Many types of everyday food are soft or can be made in soft or puréed form.